por
John R. Fischer, Senior Reporter | September 24, 2019
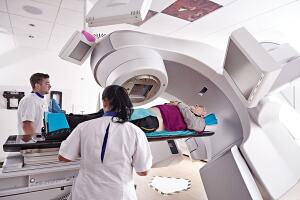
A new breath-hold technique may pave the
way for more precise and accurate delivery
of radiation to chest and abdomen tumors
(Image credit: Cancer Research UK)
Training patients about a new technique for holding one’s breath may lead to more accurate treatments and positive outcomes in radiotherapy, according to a new study.
Researchers at the University of Birmingham have developed a new method for patients to control their breathing to ensure precise targeting and delivery of radiation treatment to chest and abdomen tumors.
“There are no risks to a five-minute breath hold under carefully controlled clinical conditions. Currently patients are just asked to breath hold (a big lung inflation with room air) for about 20 seconds, then allowed to recover, then asked to breath hold for another ~ 20 seconds," Dr. Mike Parkes, a senior lecturer in applied physiology from the School of Sport, Exercise and Rehabilitation Sciences at the University of Birmingham, told HCB News. "We make the point in our paper that patients could hold twice as long if they were given 60 percent oxygen to breathe instead of air (and also were trained to inflate their lungs properly (as singers do). The real way to prolong breath hold duration however is to combine preoxygenation (inhaling 60 percent oxygen) with halving blood carbon dioxide levels."



Ad Statistics
Times Displayed: 344592
Times Visited: 21056 MIT labs, experts in Multi-Vendor component level repair of: MRI Coils, RF amplifiers, Gradient Amplifiers Contrast Media Injectors. System repairs, sub-assembly repairs, component level repairs, refurbish/calibrate. info@mitlabsusa.com/+1 (305) 470-8013
The method is based on earlier research by the team to help breast cancer patients hold their breath for five-minute periods during treatment. For abdomen and chest cancer patients, clinicians used a mechanical face mask ventilator to lower carbon dioxide levels within a patient’s bloodstream, while increasing the oxygen levels of their lungs so that they could hold their breath for four-minute periods during treatment.
Expected to make breath holds 10 times longer (more than five minutes) than currently done clinically, the approach was applied to 30 male and female cohort volunteers between the ages of 20 and 25. With practice, participants were able to hold their breath safely for longer periods of time than normal, eventually at a consistent rate of about six minutes. Researchers tested the technique in a single session by asking participants to hold their breath multiple times for four minutes. Each was hyperventilated with oxygen following a break, before resuming breath-holding. All at the end were able to hold it eight times for four minutes in a row and were able to do a final ninth breath-hold for six minutes.
The team concluded that it is both possible and safe for patients to hold their breath for about 13 minutes in three breath-holds during a treatment session just under 20 minutes, and for about 41 minutes in nine breath-holds during one of 65 minutes. Should a breath-hold have to be prematurely stopped for any reason, recovering one or more breath-holds is simple.
"I think there is still a very simple but huge self confidence issue - if staff are convinced this works and are properly trained to help patients, then it will be easy for them to convince patients that that can do it," said Parkes. "Once patients have done it once, they don’t forget (its like riding a bicycle) and it give them a huge boost to know that here is one thing they can do themselves to help their own treatment. We are currently investigating how good our technique is in patients with lung cancer and we starting to get some Industry support to help."
The use of the ventilator for helping patients control their breathing is currently being investigated in hospitals in Newcastle, and at centers in Belgium and the Netherlands.

